How Does Medical Device Injection Molding Transform Healthcare?
Walk into any modern hospital, and you'll encounter thousands of plastic components working silently to save lives. The syringe delivering medication, the catheter guiding fluids, the surgical instrument in a doctor's hand-nearly all owe their existence to medical device injection molding. This manufacturing process has become the invisible backbone of contemporary healthcare, yet most people never consider the engineering precision required to produce these life-saving tools.
The transformation happened gradually. Fifty years ago, medical devices were predominantly metal and glass, expensive to produce and difficult to sterilize repeatedly. Then came the plastics revolution, and with it, injection molding technology that could manufacture complex medical components at scale while maintaining micron-level precision. Today, the global medical device injection molding market has reached $24.3 billion in 2024, with projections climbing to $35.2 billion by 2033-a clear signal of healthcare's dependence on this technology.
Why Medical Device Injection Molding Matters for Modern Healthcare
The healthcare industry operates under constraints that would cripple most manufacturing sectors: zero-defect tolerance, absolute sterility requirements, and regulatory scrutiny that examines every molecule of material used. Medical device injection molding meets these demands through a combination of material science, precision engineering, and process control that borders on obsessive.
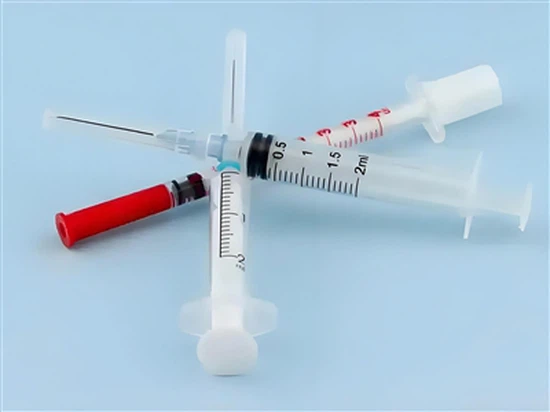
Consider the humble disposable syringe. Every day, hospitals worldwide use millions of these devices, each requiring barrel walls thin enough for visibility yet strong enough to withstand pressure, plungers that move smoothly without binding, and needle connections that never leak. Manufacturing this seemingly simple device requires holding tolerances within ±0.01mm while producing millions of identical units. Traditional manufacturing methods-machining, casting, or manual assembly-could never achieve this combination of precision, sterility, and cost-effectiveness.
The process works through controlled chaos. Medical-grade plastic pellets enter a heated barrel where temperatures reach 390-420°C for materials like PEEK (polyether ether ketone). The molten polymer gets injected into precision-machined steel molds under pressures exceeding 20,000 psi, filling cavities that may measure just micrometers across. The part cools, solidifies, and ejects-all within seconds. Modern machines repeat this cycle with such consistency that statistical variation becomes nearly immeasurable.
Breaking Down Medical Device Injection Molding Applications
Disposable Medical Devices and Single-Use Components
The disposable medical device market exploded to $113.95 billion in 2025, driven primarily by infection control concerns. Post-pandemic healthcare facilities have become even more aggressive about eliminating cross-contamination risks, making single-use devices not just preferable but mandatory in many applications.
Injection molding excels at producing these disposables economically. Take IV components-the connectors, drip chambers, and flow regulators that form intravenous therapy systems. Each component requires multiple material properties: chemical resistance to medications, transparency for monitoring, flexibility for connections, and absolute leak-proof integrity. Injection molding combines these requirements into single-shot manufacturing, producing complete parts in 15-30 seconds.
Catheters represent another critical application where medical device injection molding demonstrates its versatility. Modern catheters use multi-material molding techniques, combining rigid hubs with flexible tubing in a single manufacturing step. The hub material might be polycarbonate for strength and clarity, while the tube uses medical-grade silicone or thermoplastic elastomers for biocompatibility and flexibility. Advanced molding processes bond these materials molecularly, eliminating leak points that could harbor bacteria or cause patient complications.
Surgical instruments increasingly incorporate molded plastic components. Scalpel handles, retractor blades, and forceps tips once made entirely from stainless steel now feature ergonomic plastic grips and disposable cutting edges. A recent study documented that injection-molded surgical retractors improved handling precision by 30%, directly correlating with reduced procedure times and better surgical outcomes. The lightweight construction reduces surgeon fatigue during lengthy operations, while the ability to manufacture single-use versions eliminates sterilization failures that occasionally plague reusable instruments.
Diagnostic Equipment and Laboratory Instruments
Laboratory medicine relies heavily on injection-molded components. Petri dishes, test tubes, microplates, specimen containers, and blood collection tubes all emerge from high-volume molding operations. These items demand exceptional dimensional consistency-a microplate with 96 wells must maintain uniform depth and diameter across all wells to ensure accurate test results. Variations of even 50 micrometers can invalidate entire diagnostic tests.
The COVID-19 pandemic revealed both the importance and vulnerability of this supply chain. Testing kit components-swabs, vials, caps, and cartridges-became critical bottlenecks. Manufacturers ramped up production by running molding machines 24/7, but the precision requirements remained non-negotiable. A poorly molded test tube cap could allow contamination, rendering test results meaningless and potentially spreading misinformation about infection status.
Diagnostic device housings present different challenges. Modern point-of-care diagnostic devices-glucometers, portable cardiac monitors, rapid antigen tests-require housings that protect sensitive electronics while remaining lightweight and user-friendly. Injection molding creates these enclosures with integrated features: snap-fits for tool-free assembly, windows for displays, compartments for batteries, and mounting points for circuit boards. The housing for a typical glucometer might incorporate 15 different functional features, all molded in a single piece that weighs less than 50 grams.
Advanced Materials Driving Medical Device Injection Molding Innovation
High-Performance Engineering Thermoplastics
Material selection represents perhaps the most critical decision in medical device design. The polymer must satisfy regulatory requirements for biocompatibility (typically ISO 10993 testing), withstand sterilization methods without degrading, maintain mechanical properties across temperature ranges, resist chemicals, and often provide specific optical or electrical characteristics.
PEEK has emerged as a premium material for implantable medical devices. This semi-crystalline thermoplastic maintains properties at temperatures up to 250°C, exhibits exceptional chemical resistance, and demonstrates biocompatibility suitable for permanent implants. Spinal fusion cages, dental screws, and orthopedic plates increasingly use PEEK as a metal replacement. The material's radiolucency provides a major advantage-PEEK appears transparent on X-rays, allowing surgeons to monitor bone healing and implant positioning without metal artifacts obscuring the view.
Processing PEEK requires specialized equipment. The polymer's high melting point (343°C) and narrow processing window demand precise temperature control and high-pressure injection. Molds must be hardened to withstand thousands of cycles without dimensional changes. Despite these challenges, manufacturers embrace PEEK for high-value applications because the material enables designs impossible with traditional metals. A PEEK spinal cage can be molded with intricate lattice structures that promote bone ingrowth while reducing implant weight by 60% compared to titanium equivalents.
Liquid crystal polymers (LCPs) serve applications requiring extreme dimensional stability and miniaturization. These materials exhibit ultra-low shrinkage rates (0.1-0.3%), making them ideal for micro-molded parts like catheter connectors, sensor housings, and implantable electronics. LCP's low dielectric constant supports high-frequency medical electronics, including wearable biosensors and wireless monitoring devices. The material's excellent barrier properties protect sensitive electronic components from moisture and body fluids in implanted devices.
Biodegradable and Sustainable Polymers
Sustainability concerns are reshaping material choices in medical manufacturing. Biodegradable polymers-polylactic acid (PLA), polycaprolactone (PCL), and polyglycolide (PGA)-offer solutions for temporary implants and drug delivery systems. These materials safely degrade in the body over weeks or months, eliminating the need for surgical removal.
Absorbable sutures, drug-eluting stents, bone screws, and tissue scaffolds increasingly use biodegradable polymers. A PCL-based drug delivery implant might release medication steadily for six months before completely degrading into harmless byproducts. The injection molding process allows precise control over polymer composition and degradation rates by adjusting molecular weights and material blends.
Environmental sustainability extends beyond biodegradability. Medical device manufacturers face pressure to reduce plastic waste while maintaining sterile, safe products. Some companies are exploring monomaterial designs-single-polymer devices that simplify recycling-though regulations currently prohibit recycled materials from patient-contact applications. Energy-efficient electric injection molding presses reduce manufacturing carbon footprints by 30-60% compared to hydraulic systems, while optimized hot runner designs minimize material waste during production.

Precision Manufacturing: Micro-Molding and Miniaturization
The trend toward minimally invasive procedures drives demand for ever-smaller medical components. Micro-molding produces parts weighing mere milligrams with tolerances measured in microns. This specialized injection molding variant requires extraordinary control over processing parameters.
The medical micro injection molding market reached $596.7 million in 2024 and projects growth to $1,662.8 billion by 2033, demonstrating medicine's accelerating embrace of miniaturization. These tiny components enable breakthrough applications: intraocular lenses for cataract surgery, microfluidic channels for lab-on-a-chip diagnostics, drug delivery microneedles, and miniature surgical instruments for endoscopic procedures.
Micro-molding presents unique technical challenges. Polymer molecules must flow through channels barely wider than human hairs, filling cavities before premature solidification. Conventional injection molding relies on continuous pressure, but micro-molding often employs compressed melt dynamics-storing elastic energy in the molten polymer then releasing it as high-velocity flow when valve gates open. This technique achieves fill times of 10-20 milliseconds, creating parts with wall thicknesses down to 0.05mm.
Quality control becomes exponentially more difficult at micro scales. Traditional measurement tools lack the resolution to verify dimensions on parts smaller than grains of rice. Automated vision systems inspect every cavity twice per production cycle, using machine learning algorithms to detect defects invisible to human inspectors. A single dust particle can ruin a micro-molded part, requiring production in ISO Class 7 or 8 cleanrooms with strict environmental controls.
Regulatory Compliance and Quality Management in Medical Device Injection Molding
Manufacturing medical devices means operating under regulatory microscopes. The FDA and international standards organizations mandate quality management systems covering every aspect of production, from raw material receipt through final product distribution.
ISO 13485 establishes the quality framework for medical device manufacturers. Obtaining this certification requires documented procedures for risk management, process validation, personnel training, equipment maintenance, and continuous improvement. The standard emphasizes traceability-every component must be traceable to specific material lots, production dates, machine conditions, and operators.
Process validation represents a major undertaking for medical device injection molding operations. Manufacturers must prove that their molding process reliably produces conforming parts before commercial production begins. This involves Installation Qualification (IQ) verifying equipment installation, Operational Qualification (OQ) confirming the system operates within specifications, and Performance Qualification (PQ) demonstrating consistent production of acceptable parts over extended runs.
Statistical process control monitors ongoing production. Key parameters-melt temperature, injection pressure, cooling time, part weight-get tracked continuously with automated data logging. Any deviation triggers investigation. For example, if a molding process normally maintains a 5% rejection rate but suddenly climbs to 10%, quality systems mandate immediate investigation per ISO 13485 requirements.
The FDA's Quality Management System Regulation (QMSR) becomes effective February 2, 2026, incorporating ISO 13485:2016 as the foundation for U.S. medical device manufacturing. This harmonization simplifies compliance for companies operating globally but requires significant preparation for manufacturers not already ISO 13485-certified. The transition demands updates to documentation, traceability systems, and audit practices, with FDA explicitly noting that ISO 13485 certification alone doesn't satisfy all QMSR requirements-additional FDA-specific controls remain mandatory.
Design controls under the QMSR require full traceability between design inputs, outputs, verification testing, and validation activities. Every design decision must be documented with clear rationale and supporting data. This level of documentation ensures that if a device fails in the field, investigators can trace the root cause through the entire development and manufacturing history.
Automation, Industry 4.0, and the Future of Medical Injection Molding
Modern medical molding facilities increasingly resemble software companies more than traditional factories. Automation has evolved from optional efficiency enhancement to essential capability for meeting quality and traceability requirements.
Robotic part removal systems handle finished components without human contact, reducing contamination risks. These systems incorporate force sensors and vision guidance to detect and respond to variations in part ejection, preventing damage that human operators might miss. Touchless vacuum-based takeout systems can handle parts individually at cycle rates exceeding 20 per minute, feeding downstream operations for assembly, inspection, and packaging.
In-line inspection systems check every part against specifications. High-resolution cameras capture dozens of images per component, measuring critical dimensions while detecting surface defects, color variations, or molding flaws. Machine learning algorithms analyze these images, identifying defect patterns that human inspectors would miss. The systems can track trends across thousands of parts, predicting when maintenance becomes necessary before quality degradation occurs.
Process monitoring has become increasingly sophisticated. Cavity-level sensors measure temperature, pressure, and melt flow in real-time, generating data streams that document every molding cycle. This information feeds quality records for traceability while enabling predictive maintenance. Artificial intelligence analyzes historical data to optimize process parameters, automatically adjusting injection speeds, pressures, and cooling times to compensate for material variations or ambient condition changes.
Digital twins-virtual replicas of physical molding processes-allow engineers to simulate production scenarios without consuming materials or machine time. These models predict how design changes or new materials will behave before committing to expensive prototype tooling. Simulation software can predict weld lines, air traps, warpage, and other defects, enabling designers to optimize part geometry for moldability.
Cleanroom Manufacturing and Contamination Control
Medical device production often requires cleanroom environments where particle counts, temperature, humidity, and airflow receive continuous monitoring and control. ISO Class 7 cleanrooms (10,000 particles ≥0.5 micrometers per cubic meter) provide the standard environment for most medical molding operations, while more critical applications demand ISO Class 6 or even Class 5 conditions.
Maintaining cleanroom integrity while operating injection molding machines presents challenges. The machines generate heat, particles, and vibration-all enemies of contamination control. Purpose-built cleanroom presses incorporate features like HEPA filtration on exhaust ports, enclosed tool areas, and low-particle generation components. Personnel entering cleanrooms undergo gowning protocols, wearing full-body suits, gloves, and face coverings to prevent shedding skin cells or fibers that could contaminate products.
Even the molding materials require special handling. Medical-grade resin arrives in sealed, certified lots with extensive documentation. Raw material gets dried under controlled conditions to eliminate moisture that could cause bubbles or surface defects. Material handling systems convey resin from storage to molding machines through closed pathways, preventing exposure to room air that might introduce contaminants.
Assembly and packaging operations that follow molding face even stricter requirements. Devices often undergo ultrasonic or laser welding in cleanrooms to create finished assemblies, then move to sterile packaging lines where every seal gets verified. The entire production flow from raw material to packaged device happens in controlled environments, with multiple inspection points ensuring no contamination opportunity exists.

Economic Impact and Market Dynamics
The medical injection molding sector demonstrates remarkable growth across global markets. North America dominates with 40% market share, driven by advanced healthcare infrastructure and high per capita spending. The region's aging population (projected to reach 1.4 billion people aged 60+ by 2030) creates sustained demand for medical devices and disposables.
Asia-Pacific represents the fastest-growing market, with projected CAGR exceeding 7% through 2033. China, India, and Japan invest heavily in healthcare infrastructure, building hospitals and expanding medical services. As an example, India plans to add over 20,000 hospital beds in the next five years through projects like the 750-bed Rewari AIIMS Medical College, the 4,000-bed LNJP Hospital expansion, and multiple 1,000+ bed facilities. Each new hospital requires millions of injection-molded medical products-from examination gloves and specimen containers to sophisticated surgical instruments and implantable devices.
Material costs significantly impact economic calculations. High-performance polymers like PEEK cost two orders of magnitude more than commodity plastics like polyethylene. A kilogram of medical-grade PEEK might cost $150-200, versus $2-3 for polypropylene. This creates strong incentives to minimize material waste through optimized hot runner systems and precise process control. Manufacturers invest in simulation software and advanced tooling to reduce scrap rates from 5-8% down to 1-2%, saving thousands of dollars annually on high-value materials.
Tooling represents another major investment. A precision mold for medical components might cost $50,000-250,000 depending on complexity, number of cavities, and material requirements. Multi-cavity molds amortize this investment across higher production volumes, but validation requirements mean the tool must produce conforming parts consistently before production authorization. Failed tool validation can cost months of delays and hundreds of thousands in redesign expenses, making upfront engineering investment critical.
Real-World Applications and Case Studies
Orthopedic surgery has embraced injection-molded PEEK implants enthusiastically. A typical spinal fusion procedure now uses PEEK cages molded with porous surfaces that encourage bone ingrowth. These implants weigh 60% less than titanium equivalents while providing comparable strength. The radiolucency allows surgeons to verify fusion progress on post-operative X-rays without metal artifacts obscuring the view. Clinical outcomes show faster patient recovery and fewer complications compared to metal implants, driven partly by PEEK's elastic modulus matching natural bone more closely, reducing stress shielding effects that can weaken surrounding bone.
Wearable health monitors represent another growth area. Devices like continuous glucose monitors, ECG patches, and biosensors require housings that protect electronics while maintaining comfortable contact with skin. Injection molding creates these enclosures with integrated features: battery compartments, sensor windows, adhesive mounting surfaces, and snap-fits for assembly. The parts must withstand body heat, moisture, and movement while remaining hypoallergenic and comfortable for 24/7 wear. Thermoplastic elastomers (TPEs) provide skin-friendly surfaces that won't irritate during extended contact.
Microfluidic diagnostic devices showcase micro-molding capabilities. Lab-on-a-chip platforms integrate sample handling, reagent mixing, and detection in credit-card-sized devices. These systems contain networks of channels, chambers, and valves measured in micrometers, all molded in single operations. Point-of-care diagnostics for infectious diseases, cardiac markers, and metabolic panels increasingly use these platforms, enabling rapid testing in physicians' offices, ambulances, or patients' homes. The technology proved crucial during COVID-19, accelerating test result turnaround from days to minutes.
Frequently Asked Questions About Medical Device Injection Molding
What makes medical injection molding different from standard plastic molding?
Medical molding operates under FDA and ISO regulations requiring validated processes, complete traceability, biocompatible materials, and cleanroom manufacturing. Every production parameter gets documented, and any deviation requires investigation. Standard molding focuses primarily on dimensional accuracy and appearance without the extensive quality systems medical applications demand.
How long does it take to develop a medical injection molded device?
Development timelines vary significantly based on device classification and complexity. Simple Class I devices might progress from concept to production in 12-18 months. Complex Class III implantable devices require 3-5 years for design, testing, clinical trials, regulatory approval, and manufacturing validation. Tool development alone typically takes 12-16 weeks once designs freeze.
Why are medical-grade plastics so expensive?
Medical-grade resins undergo extensive testing for biocompatibility, extractables, and leachables. Manufacturers maintain strict process controls and comprehensive documentation. Batch-specific certificates of analysis accompany every material lot. These quality systems and testing protocols increase costs significantly over commodity plastics, but ensure materials won't harm patients or compromise device function.
Can injection molded medical devices be sterilized?
Yes, most medical plastics withstand common sterilization methods including steam autoclaving, gamma radiation, ethylene oxide gas, and electron beam treatment. Material selection considers sterilization requirements-some polymers degrade under specific sterilization methods. Devices intended for reuse must endure multiple sterilization cycles without property degradation.
What's the difference between medical molding and cleanroom molding?
All medical device molding requires quality systems per ISO 13485, but not all occurs in cleanrooms. Devices that don't contact patients directly-housings, external enclosures-may be molded in standard manufacturing environments. Components that contact sterile body areas, implants, or disposables for fluid handling typically require cleanroom production to prevent particle contamination.
How does automation improve medical device manufacturing?
Automation eliminates human contact with products, reducing contamination risks. Robotic systems handle parts more consistently than manual operators, improving quality and reducing rejection rates. In-line inspection catches 100% of defects versus statistical sampling. Data logging documents every molding cycle for complete traceability. These capabilities prove essential for meeting regulatory requirements while maintaining economic viability.
What role does 3D printing play in medical injection molding?
Additive manufacturing enables rapid prototyping in actual production materials, accelerating development cycles. Designers can evaluate multiple design iterations quickly before committing to expensive production tooling. Some companies use 3D-printed molds for low-volume production or initial clinical trials. However, 3D printing currently cannot match injection molding's precision, surface quality, or cost-effectiveness for high-volume medical device production.














